Friday, August 21, 2015
孩子,你慢慢来 (Because I Love You) TV Documentary
It is a 4 episode series featuring babies/toddlers who require special care.
This documentary series was aired on Channel U
Kaelyn initially wasn't supposed to be featured that much but for some reasons, she got more involved and was featured much more than we had expected.
She passed away 4 days after her final filming session.
Grateful for the production crew and the chance that Kaelyn got her story told.
The YouTube links are below. For some reason, some portions of the videos are silent or lack background music, which are not production fault.
Episode 1
Episode 2
Episode 3
Episode 4
HCA Remembrance Day Sharing
This is a day where they remember the sons and daughters under the care of Starpals, who have earned their wings.
======
Kaelyn will be 3 1/2 years old exactly tomorrow. However she isn't around anymore.
She passed away on April 23rd 2015 due to Spinal Muscular Atrophy Type 1.
We have been invited to share abit on this day as we remember our kids who have been around.
Discovery of her illness
Kaelyn was born normal but at age 6 months, we were told she have muscular atrophy type 1 by a neurologist.We didn't know what it was. We went home checked the Internet about SMA Type 1. It sounded and is horrible and terrible as those affected will lose control of their muscles and will atrophy.
Anything that requires muscles will be affected. From sitting, moving and even breathing.
And her symptoms totally fit.
We were devastated even though the results had not come back. We waited for 2-3 weeks for the result to come back.
Grief
We grieved about her diagnosis. It was like a death sentence for her. We've been through the stages of grief.Denial
We try to tell ourselves it may be other reasons why she is so weak.How can it be this genetic disease when we do not remember of any family history.
We keep thinking she could be slow in development. Or she is taking her time to grow stronger.
Anger
Then we were kind of angry. How could it be? Who could play such a joke on us.Bargain
Can I give up years of my life for a normal life for my girl? Pretty please whoever is up there.Depression
Whenever we thought of her diagonsis, we would tear up. Why does this little child of mine have to suffer from such a disease.After 2-3 weeks of waiting, we received her result. We cried and cried that day.
Acceptance
But that was the day when we tell ourselves that Kaelyn young as she might be, will know and feel the mood.We shouldn't let her think that why is she always making her mummy and daddy sad.
We told ourselves that we should simply keep her happy, and at the same time treat her as normal kid as much as we can.
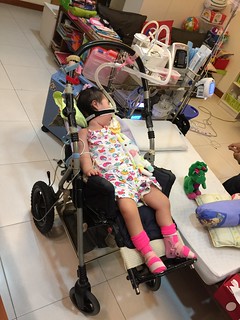
Our daily life
Take away the BiPap, milk pump and other equipment, She is just a normal little girl.She wants to munch on food, even when she is tube fed from 10 months old onwards.
She wants to watch her TV shows.
She loves dolls.
She loves to paint her nails.
She loves to go to the playground. And she throws tantrum if she feels she haven't spend enough time at the playground.
Insert medical emergencies now and then, and physio session everyday, we try to give her a normal life.
As long as she's happy. We told ourselves.
Lesson learnt
In the documentary where Kaelyn was filmed. We were asked if we've learned anything.I did not really have an answer. As it happened quite fast
But we think now we have.
Think positive
We are encouraged by her positive outlook of her life.She has been tube fed for most of her life.
One day at the playground, we asked her if she wants porridge when we get back home, she did a HAHA! Because she knew she is tube fed so no porridge for her.
At the playground, she is very content to watch kids play. Though I believe she deeply desires to be able to run up the slides, slide down, and then do it repeatedly.
You could say this was the only life she had. Immobile and tube fed. But we cannot deny that she has a always been cheerful and contented most times of her life.
Sharing and encouragement
Kaelyn most times is willing to share what she has, or what she knows.In one of the hospital stay, Kaelyn was going to do her chest physio and cough assist.
A young doctor happened to be around and asked what's a cough assist.
Mummy asked her, Doctor don't know what's a cough assist. Can you show him how we use it?
Kaelyn answered loudly yes! She went on bravely to do her coughs and suctions, as if she was doing a product demonstration.
We were encouraged by her to share her story to encourage anyone in a similar boat.
Her passing
Her deterioration came as sudden as lightning. After few days in ICU, We had to let her go.We had been mentally preparing for such a day to come. But when it came, we still weren't prepared.
It's like we had a dream of 3 years 2 months and 7 days.
A poem I came across, Author unknown
A butterfly lights beside us like a sunbeam
And for a brief moment its glory and beauty belong to our world
But then it flies again and though we wish it could have stayed...
We feel lucky to have seen it.
Closing
On this day, we remember our little angels, who have departed prematurely in their lives.Ultimately, their lives are much shorter than normal.
How long? we don't know at that time. We know we just want our kid to be happy.
Though unwilling to be apart, we rejoice in the hope that Kaelyn has a whole body, and is free from the shackles of her old body. Now she is free to run, hop and play.
Thursday, May 14, 2015
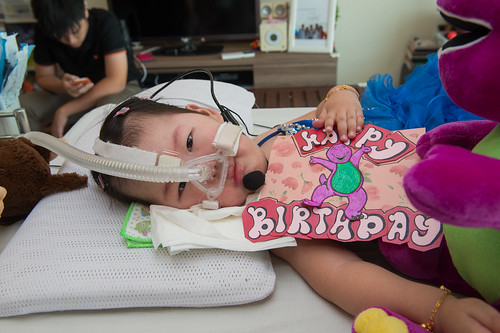
One of the early celebration for Kaelyn's 3rd Birthday
One of the few celebrations we had for her birthday. Happy times...
Tuesday, May 5, 2015
Epilogue - Kaelyn's Journey
There is no beeping sounds from the oximeter, humming sound from the oxygen concentrator or sound of air gushing through the BiPap machine.
The most significant absence is the sound of Kaelyn and mummy's playtime, the constant bantering between Kaelyn and our helper whenever they are together, and Kaelyn calling me as I walked past her room to mine to drop my stuff down after work.
This is the new usual, it seems.
It all seems like a dream.
We bade farewell to Kaelyn almost 2 weeks ago. She earned her angel wings.
Though the journey with her short, it was also intense.
Her diagnosis of SMA Type 1 at that time was like a bad dream.
But I do know the time spent together is very real.
Since her diagnosis, we have tried our best to keep our promise of keeping her happy for as long as she lives.
We are prepared for this day to come, but we are never ever prepared.
Until her last conscious day, she was still cheerful and playful as always.
She remembered all the story telling, dancing moves and the singing by those that drop by and visit her. She loved it all.
She really digged the photo shoot by Portrait from the heart. She wasn't fussy and in between shots she would take a break, just like a diva would, except she puts on her BiPap for some breath and to clear her secretions, then snap some photos once more.
Most importantly, that was our only proper family portrait, which we cherish it dearly.
When she was well few days before the acute incident, we've contemplated about few issues on change of a different feeding tube, quality of life issues and her comfort.
Our helper was thinking of heading home and ending her contract at year end. That will need mummy to stop work and/or find a suitable helper to hire at home.
No firm decisions were made at that time.
Kaelyn is always decisive about her choice of playtime, clothes to wear or cartoon to watch.
On one warm day after her bath, she decided it was too warm to put on clothing. she FaceTime her noon time call list, wearing only her diapers, and seemingly proud of her playful defiance.
This time round, just like her normal feisty self, she seem to choose her way.
There was no need for anyone of us to make up any decision for her.
And it seems like this was actually the best way for her, judging from all the circumstances.
When well, Kaelyn regularly goes to the playground below the block and just look at the kids play.
Occasionally, she wants one of us to play on the swing or work out on the exercise station. It is as if she does what she wants to do through us.
You have always yearn to play on the swings and merry go rounds in the playground.
It has been tough on Kaelyn physically, but she has endured it all, always coming out of situations with smiles and cheerfulness.
I was wrong. You have been brave. You have been a fighter.
Your fight is over now. You have broken free, and with a complete body. Go now girl (still my baby), have an adventure of your own.
Tuesday, April 14, 2015
We don't wish to but we have to
I had to drop by the hospital as I have arranged to meet the parent of Chloe to pick up some things.
They are one of the family in our support group.
I was there as the nurse was attempting to set the IV plug on the wrist for Chloe’s treatment.
This is a weekly event for Chloe.
The nurse tried 2 or 3 times to find the vein but couldn’t.
I left. But they did eventually set the plug successfully on the other arm
I thought of Kaelyn resting at home nursing her infection. It’s been 12 days since she started having intermittent fever.
We are contemplating hospital admission but don’t wish to risk any other form of infection (although you could say she already is)
We have increased the intensity and occurrence of her chest physio daily in the attempt to keep her lungs clear and open as her mucus generation increases following the onset of some form of infection.
When she’s sick, her schedule are like this 1. Wake up 2. Start nebulizer 3. Chest percussion (this could take awhile) 4. Cough assist and suctions 5. Rest/play 6. Nap
Repeat the above for 3 times during the day time.
Our coughs, percussion and suction could take quite a while (as long as 2 hours sometimes) as we try to clear her airways properly.
We jammed up 3 suction catethers attempting to clear her single nasal airway yesterday. It was thick and sticky even after the nebs.
The treatment/therapy takes out a lot from Kaelyn. She looks dead beat after that.
As a parent, I believe it hurts for parents to see their child go through such pains of probing and piercing, let alone on a regular basis.
We could only try our best to console the kid as they undergo the treatment/therapy to get them better.
Making them undergo treatment/therapy are sometimes between the devil and the deep blue sea.
If only pain is transferable.
We don’t wish to but we have to. Sigh.
Note: I understand there are individuals that may ask why put them through more pain in their life. Of course this question definitely comes to the mind of the parents of special needs kids. But that would be another topic for another day :)
Thursday, March 26, 2015
da da ma ma
Mummy’s with her.
She grab mummy’s attention with her vocable call for attention. Mummy asked if someone walked past the room.

She answered yes.
Mummy asked who was it?
She managed to vocalized “da-da”
We tried that a few times of me walking by and Kaelyn calling out and identifying who walked past.
Then I switched role with mummy.
She manage a “muaaa”
Later I told her to try this “muahahahha”, something like Dr. Evil’s laughter.
She did a “muaa. Haha”
ROFL literally.
Her body is limiting everything a human can do. Even the muscles to smile is diminishing. When smiling she could only manage to curl one side of her lip up.
It’s really nothing to scream about for a 3 year old to barely make phrases or speak the words that resonates with just ahhs but inside us, we are squealing with delight for Kaelyn.
Friday, March 20, 2015
an earlier home care appointment
We brought Kaelyn to her home care appointment last Friday. It’s her first time out of the house since last December (not counting trips to the A&E)
It was supposed to be 2 weeks later but it has been an eventful month (here and there). Home care and Starpals team deem it significant to bring forward the appointment.
Mandatory for every visit. The weigh in of daddy and Kaelyn. We totaled almost 100kg(97kg). We both grew in weight! Kaelyn was almost 15kg
I think she grew in her height too at 103cm.
There were discussions which mainly focus on her current main risk now, which is aspiration.
Recommendations were thrown in 1. Change to a faster absorption milk feed 2. Change to a GJ feeding tube
We are leaning towards option 2 ultimately as option 1 is a may/may not help.
However the frequent reports of bursting of the current batch of GJ tubes worries us.
Monday, March 2, 2015
Rude awakening
She looks like she was in discomfort. We went through part by part asking if this was painful. she said her stomach was aching. We had to suction her thick secretion present in her mouth.
It wasn’t the 1st time tonight she had to wake up and be suctioned. I was too deep in the sleep to hear what’s going on.
We cleaned her, settled her down and stabilized her and everyone tried to went back to bed.
Another shout.
This time she was aspirating. One of the worst fear we have.
My helper was suctioning. Had to bag her for a while. Managed to clear her airway and pacify her to rest without more drama.

Let’s hope no more drama
Kaelyn aspirating isn’t the first time within a short time frame.
It seems it happens when her body is stressed. It may be a sign of fundoplication becoming loose.
Right now K is knackered and is asleep with higher than usual heart rate. The oxygen concentrator is still humming away, providing O2 for her.
I couldn’t rest now, but just wondering…
How could we do without the oxygen concentrator for 2 years?
Silly me. By running to the hospital every time shit like this happens.
Both hospital and us could save more money by making this a subsidized standard item for special needs kid like K in the beginning. We save on hospital trips. They save on subsidies. They just need to prevent us from going to hospital 1 time less to cover the cost.
PS Just going off tangent wildly on the last part. Silly sleepy brains not going to sleep but having silly thoughts now.
Friday, February 27, 2015
3 not so easy years
First one was with a volunteer and her friends, where Kaelyn got serenaded with singing from the visitors.
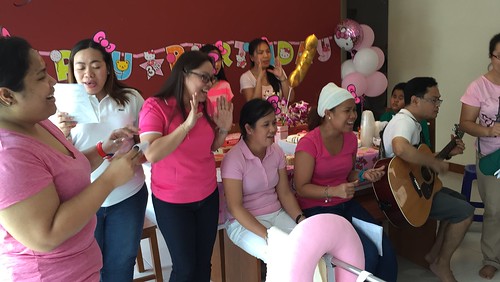
The 2nd was with immediate family members where Kaelyn was a princess for the day.
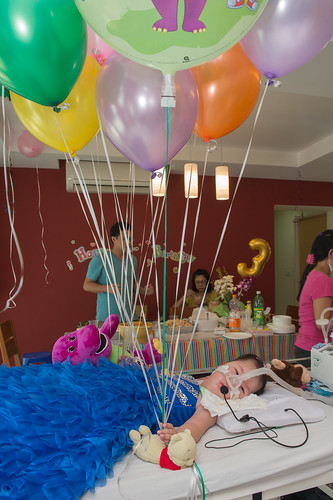
Every year is worth a celebration considering 2 years is the average lifespan for SMA Type 1 kids.
I think for them to wake up and breath everyday is a miracle for them.
The simplest task of swallowing water could choke them.
The suit of Darth Vader probably don’t help much.

There are ups and downs. The bad days life threatening, while the the ups are simply having fun days that puts a smile on K’s face (and without any choking or mucus pluggin episodes) and we treasure that.
The highlight of last year was of course the trip on the cruise. Kaelyn absolutely loved it. It sure took quite an effort on the logistics part.
We were also faced with literal life or death decisions yet again in the wards of the ICU, where we contemplated hard about Kaelyn’s life, death, quality of care and comfort.
We are thankful that we didn’t have to go through with our worst case scenario decisions.
Every checking out from a critical stay in the hospital feels like a student just scrapping pass the exams. Just barely made it.
We made it through another year. But we have to be realistic. But as much as we want to, for now, we cannot beat SMA.
In fact at any time, if a mucus plugs her airways or she aspirates her feeds, her life will be in danger if we are unable to clear it in time for her to breathe.
But for now, we celebrate the days. We try to lead an inclusive life with Kaelyn with the support of friends and family (even strangers for that matter) and face the challenges of a special kid.
Monday, February 9, 2015
A helping hand

It reminded me of the time when we just discovered that Kaelyn’s journey is going to be different.
I supposed you could say it was dark days.
What to do? We didn’t know the when, whats, hows and why.
We could only turn to the Internet. We found articles writing about SMA being the number 1 genetic baby killer, does not live pass 2 years, no cure. It was depressing.
We found the Muscular Dystrophy Association Singapore (MDAS). Sent an email in asking for any help but was expecting my mail to be lost in the imaginary heap of mails that is the enquiries mailbox.
But we did get a reply and they linked us up with parents who were willing to share their experience with us.
Fredrick and Rebekah was one of them. They let us visit them and they shared their experiences of their own. Their younger daughter, Danielle, also has Spinal Muscular Atrophy (SMA).
It sure helps with a helping hand, especially one who have walked through the road we have to take.
Thursday, February 5, 2015
Just some bad days
Kaelyn heart rate was tachy and wasn’t holding her spO2 too well this evening.
We didn’t finish her sets of cough assist. We gave her a break after checking that she sounds clear enough.
She just wasn’t holding it too well today.
Seems like she’s like this when she doesn’t get enough rest.
Last Saturday was more stressful.
Same thing. Tachycardia and spO2 didnt hold up well. She even seem to aspirate her feed.
Aspiration of her feed is bad as it could go into her lungs and lungs could collapsed.
SpO2 dropped well into the 50s% (healthy is 95% and above)
We standby to bag her on Saturday. But we didn’t have to. Good not to stress her body further.
After her own record ICU stay, she’s really more fragile.
Her fingers weaker.
Ankles stiffer.
Her smile is fading.
Her voice lacking her usual strength.
The combination of the progression of her disease, splints preventing her hand movement, IV lines preventing her wearing of her AFOs just takes the poll on her.
I go to bed thinking when she recuperates enough, maybe she can wave her hands, give me a bigger smile and shout so loud from the hall, I can hear from the corridors when I come back from work.
Just a weak maybe.
She’s in good spirits most times, but it just takes lesser to set her off now.
if she starts to not have quality naps and night sleep, She is literally alarming. Her heart rate goes up to 180–190 like a sports car going into the highway and her spO2 goes below the healthy level and stays there long enough for you to worry.
It’s like screw it, I am tired breathing normally. Take 5. Breath harder in awhile. Let them go fix me a dose of O2 therapy for me. Chop chop.
We scramble around, put her into her favorite position, suctioning what we could suction, supplement whatever appropriate dose of O2 she needs.
Amidst the frantic action going on, We tell her It’s ok baby. Rest and relax, but just remember to breath in breath out.
As K’s previous therapist told us, We are going to have just some bad day now and then (somewhere along that line)
Just some bad days.
Thursday, January 22, 2015
Out of hospital
3 weeks ago we admitted her into the hospital We have had difficulties managing her secretion and mucus while in the High dependency ward after almost a week and had to bring her to the ICU, put in the ETT.
Tuesday, January 13, 2015
Turn of event
Her fever spiked. It’s not high but it’s a constant low grade fever.
Her secretions and mucus became more in volume. Together with bleeding in her nose and throat (probably trauma from suctioning), all these just stuck together, making things unmanageable.
We were literally fishing for mucus plugs.
We bagged her few times.
We were recommended to intubated her. We went ahead with that to make her breathing and secretions more manageable.
Being intubated, she is now in ICU. Fever is gone.
We took the chance to do a bronchoscope procedure, clearing a plug in the airways Where we wouldn’t be able to reach it.
Her secretions production still high gear. We have still been able to keep her lungs clear, a plus point.
We are awaiting for better, clearer conditions in her airway to extubate her.
Gosh this feels like a rocket launch.
Fingers crossed
Wednesday, January 7, 2015
Not a start to the year we want
Not a start we want for the year, month, week, day or hour as a matter of fact.
We arrived into the hospital, after bagging her, in an ambulance.
We were doing music therapy and she was humming along. Then suddenly she turned quiet, gave non-responsive stare and her sats just plummets.
We stablised her after a while but the ambulance was well on its way.
For the past few days, she has fever that goes up and down for the past few days. Her inside of her nose is also swollen and bloody after numerous suctioning to clear her airways.
Her condition is stable so far.
I sit here writing this and having second thoughts, such as we probably shouldn't have needed to leave home if we handled the situation better.
We should be more confident in our knowledge of K's condition and whatever life saving hacks for K.
After all, if possible, home is the best for resting and recuperating.
The first night, we had a boy opposite us who couldn't stop crying. No rest for that night.
The hourly checks for temperature and blood pressure in the day and night just irritates K out of her rest.
The aircon went bonkers as well, rendering the ward as cold as a data centre server room temperature. This also had some effect on K's sleep.
But on 3rd thoughts, we are kiasee :P Scenarios like bagging her halfway and we run out of oxygen and then not sure how to sustain her in the last minute dash to the hospital.
After the incident and admission, I had a chance to talk to a doctor who knows K and her condition. We talked and walked thru about what had happened and he gave some information on what usually will happen during sickness and the effect it has on kids with compromised breathing.
We take this as a lesson that we need to MENTALLY rehearse (we do not want an actual situation again ever!) well to handle well such emergencies, that will take place so often on kids with Spinal Muscular Atrophy.